by Joyce Warner
Transcript for Video
[Video Start]
[Video presented with written slides in English]
[music]
[FEEA #FEDLIFEHACKS logo with a light bulb at the top encased by a blue box.]
[an image of the legs of three women of various ethnicities.]
Keeping Your Skin Healthy
[An image of a mother putting sunscreen on her daughter’s face.]
How to use sunscreen:
- Look for SPF 30 or higher
- Apply 15 minutes before sun exposure and reapply about every two hours
- Seek shade, wear protective clothing, and be extra careful/avoid exposure from 10am - 2pm
[An image of an African American man watering his lawn.]
Besides sunscreen, how else should we protect skin this summer?
- Wear gloves when gardening or doing yardwork
- Use insect repellant
- Stay cool, dry, and hydrated
[an image of a tick on a microscope.]
What about other outdoor-related issues?
Lyme disease and other tick-borne illnesses can be dangerous and have long-lasting effects. Carefully check yourself, children, and pets after being outdoors.
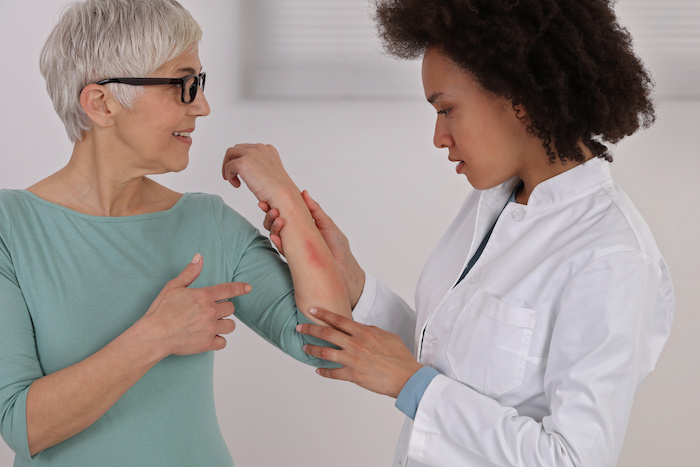
[An image of a female African American doctor checking a rash on a female Caucasian]
When should you see a doctor?
- Any new rash, especially if accompanied by fever, muscle aches, joint pain, and/or headache
- Unexpected darkening or lightening of skin
- Other new changes, like acne or hair loss can also signal underlying conditions
[An image of hands and arms of various ethnicities interlocked and forming a circle]
Hand dermatitis (dry, itchy skin) from frequent washing and sanitizer use is becoming more prevalent. To combat, limit hot water use, avoid harsh soaps, and moisturize after washing.
for more information on this topic, visit feea.org/skin
[Blue Cross Blue Shield Federal Employee Program Logo.]
FEEA thanks BCBS for contributing to our #FedLifeHacks program
[FEEA #FEDLIFEHACKS logo with a light bulb at the top encased by a blue box.]
[music]
[Video End]
I recently sat down with Dr. Lane Neidig of Advanced Dermatology to talk about skin health. The summer is a popular time to talk about skin (the largest organ of the body), but it’s something we need to pay attention to year-round.
Joyce: Dr. Neidig, thank you so much for joining us today to talk about skin health. It’s summer, so we should start by talking about the sun, insects, and plants that can cause skin ailments and damage. What are the best ways to protect yourself and your children outdoors this summer?
Dr. Neidig: Protecting our skin is a year-round task with summer being the most important time to protect our skin from excess heat, sunlight, and the great outdoors. Chronic sun exposure can cause pre-mature aging of the skin and increases the risk of developing skin cancer. Sunlight can also cause exacerbation of acne, rosacea, and other photosensitive conditions such as lupus.
It is important to utilize insect repellant and avoid walking in areas of high grass with exposed skin to avoid ticks and mosquitoes. When performing yardwork, it is important to wear gloves and cover exposed areas to avoid injury from thorns or exposure to plants such as poison ivy.
Exposure to excess heat can also worsen existing rashes such as eczema or produce heavy sweating leading to superficial skin infections due to the overgrowth of yeast or fungus. It is important to stay dry, cool, and hydrated during the summer months.
Joyce: Since wearing sunscreen year-round is a recommendation we hear often; can you share what to look for in a sunscreen and how often it needs to be applied/reapplied?
Dr. Neidig: The American Academy of Dermatology recommends the application of broad spectrum SPF 30 or higher to all exposed areas. When applying sunscreen, do so 15 minutes prior to going outside and apply a thin layer of coverage. It is important to reapply about every 2 hours with some brands recommending reapplication every 90 minutes. It takes about one ounce (the size of a shot glass) to apply a thin layer of sunscreen to the full body of an average adult. Even though sunscreen is effective, the gold standard of sun protection is to seek shade, wear sun protective clothing, and avoid direct sun exposure especially during the hours between 10:00 AM and 2:00 PM.
Joyce: Have there been any changes over the last few decades in the prevalence of certain outdoor-related skin conditions and illnesses?
Dr. Neidig: We have seen increased numbers of tick-borne illnesses such as Lyme disease in endemic areas such as the Northeast. Other tick-borne illnesses are also on the rise for reasons not fully understood. Tick-borne illnesses can have effects on the internal organs or joints if left untreated. The importance of doing routine tick checks on adults, children, and pets cannot be overstated.
The rates of skin cancer have been increasing in incidence over the past few decades. The most concerning of these being the increased incidence of melanoma, one of the most dangerous types of skin cancer. It is more important than ever to make skin protection a priority to prevent the future risk of skin cancer. Obtaining a baseline skin check and following the recommendations of your board-certified dermatologist is always a good place to start.
Joyce: I know sometimes skin complaints can be representative of broader health issues that extend beyond the skin (for example Lyme disease). What are some other symptoms someone should be on the lookout for and when should they see their doctor or seek immediate medical help?
Dr. Neidig: The skin is the largest organ in the body and can frequently show signs of underlying systemic disease. Any new rash accompanied by systemic symptoms such as muscle aches, fever, joint pain, or headache should always be urgently evaluated by a medical professional. Some rashes can be from infections with significant consequences if left untreated and undiagnosed.
It is also important to seek evaluation when noticing changes in your skin that are new. For example, the onset of acne or hair loss can often be a sign of underlying hormonal dysfunction in patients. The darkening of skin around the neck can be a sign of insulin resistance and pre-diabetes prompting interventions such as diet and exercise. Skin eruptions can also be due to the use of common medications such as antibiotics, over-the-counter medications, and medications for high blood pressure. Your dermatologist can be very helpful in teasing out which of your medications may be responsible for your rash.
Joyce: What about common nail and hair conditions? Any prevention tips for specific areas?
Dr. Neidig: One of the most frequent hair conditions we encounter is alopecia, the medical term for hair loss. It is important to have this evaluated early to obtain a diagnosis before significant hair loss takes place. It is always abnormal to have burning, pain, tenderness, or itching in the scalp, especially when accompanied by hair loss. This should be evaluated and treated by a board-certified dermatologist to start treatments and prevent the possibility of permanent hair loss.
The most common nail condition we see is called onychomycosis, the fungal infection of the nails. This presents as thickened, yellow, or discolored toenails or fingernails and is usually accompanied by a build-up of debris under the nail. Treatment of fungal nail infection is difficult and can include prescription nail lacquers, solutions, or oral anti-fungal medications. Treatment is usually effective but recurrence rates are high. It takes up to six months to grow a fingernail and up to a year to grow a toenail – so patience is key.
Joyce: Are there other common skin ailments you see in your practice these days? Can you share some suggestions for prevention of these medical issues?
Dr. Neidig: I frequently see hand dermatitis exacerbated by frequent hand washing, sanitizer use, and work-related use of gloves. Hand dermatitis can initially start as dry and cracked skin which then progresses to bumpy or itchy patches of skin on the hands or side of the fingers. In order to prevent hand dermatitis, we recommend limiting hot water use, avoiding harsh soaps or scented products, and moisturizing the hands after washing. If rash or itching persist despite these efforts, you may need evaluation to determine the need for prescription topical anti-inflammatory medications or potential testing to rule out dermatitis due to contact with allergens or irritants.
More from FEEA
Subscribe to FEEA’s Newsletter
FEEA thanks BCBS for contributing to our #FedLifeHacks program
The information provided in this piece is for your convenience and informational purposes only and not to be construed as professional advice. FEEA and its coauthors and sponsors are not liable for any losses or damages related to actions or failure to act with regard to the content in this piece.
Would you like to reprint this piece in your agency human resource, federal employee association, or union local newsletter? You can do so at no cost by contacting admin@feea.org with your request.